Introduction
Dental radiography plays an important role in the initial diagnosis and further treatment plan in routine dental practice. Usually orofacial pathologies are diagnosed on the basis of clinical, radiographic, and histopathological examination. Drawbacks arising in conventional 2D radio-graphy can be offset by using three-dimensional imaging, i.e. cone beam computed tomography (CBCT). CBCT is a three-dimensional imaging modality that helps in the precise determination of the extent of lesions of orofacial structures and is quite helpful in the detection of odontogenic and non-odontogenic pathologies [1].
Recent CBCT systems with reduced radiation exposure, giving high-contrast images that are almost equal to bone window computed tomography (CT), have resulted in an increase in the indications for CBCT application in the evaluation of bone density assessment, complex diagnostic and treatment planning, surgical assessment of pathology, and much more [2,3].
Greyscale in CBCT is the ability of a scan to display differences in attenuation of radiation beam. This parameter is called the bit depth and it determines the number of shades of grey available to display the attenuation i.e. to detect the subtle contrast differences. The greyscale value or voxel value is the attenuation number of a particular matter, which is based on the density of the structure [1,4]. The use of CBCT as a delineating imaging modality for different osseous pathologies has been reported in very few studies [1,2,5-7].
Thus, the use of the greyscale value in assessing the internal tissue changes associated with osseous lesions of jaws can be of great help in posing the near final diagnosis or differentiation of different osseous lesions.
Material and methods
This was a retrospective study conducted in the Department of Oral Medicine and Radiology of the Dental Institute after obtaining the approval from the Ethical Committee. Previously available CBCT scans meeting the criteria were included in the study. Inclusion criteria included the following: CBCT scans of benign osseous lesions (cyst/tumour/tumour-like lesion) with confirmed histopathological reports. Exclusion criteria included the following: CBCT scans with blurred or distorted image and scans not accompanied by complete histopathological report.
A total of 72 CBCT scans were evaluated using a SIRONA ORTHOPHOS XG 3D machine with 8 × 8 cm field of view (FOV). While interpreting the CBCT scans the following routine radiographic parameters were exa-mined for each lesions: location, periphery and shape, internal structure, and effect on surrounding structure. All the scans were divided into two groups based on the histopathological reports:
group A – histopathological reports confirming cystic lesions (n = 39),
group B – histopathological reports confirming tumour or tumour like lesions (n = 33).
The greyscale measurements were done on axial section of CBCT. For analysis of the grey values, the epicentre of the lesion was evaluated. The intersection of two perpendicular lines at the centre of the lesion was considered as the epicentre, as shown in Figure 1.
Figure 1
Cone beam computed tomography scan showing axial sections of two benign osseous lesions for the measurement of grey scale value at the epicentre of the lesion
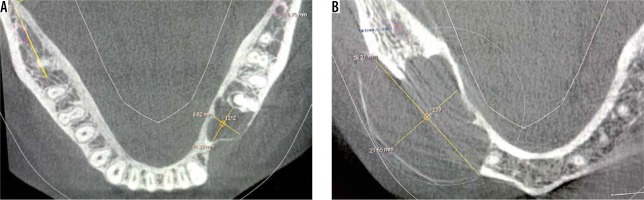
All the values were noted and tabulated to obtain the range for both the groups.
Data analysis
Data were analysed using Statistical Package for Social Sciences (SPSS) version 21, IBM Inc. Descriptive data were reported for each variable. Descriptive statistics such as mean and standard deviation for continuous variables and frequency along with percentages of categorical variables were calculated. A bivariate analysis was performed using independent t test. The level of statistical significance was set at p less than 0.05.
Results
In this cross-sectional study, a total of 72 CBCT scans along with the details showing osseous pathologies were obtained from the previous database. The age of the patients ranged from 10 to 84 years, with a mean age of 51.55 years (Table 1). Out of these 72 patients, 37 were male and 35 were female. In group A, 23 scans (58.97%) were of males and 16 scans (41%) were of females; the male to female ratio was 1.4 : 1. In group B the ratio was 1 : 1.3, in which 14 (42.4%) scans were of males and 19 (57.6%) scans were of females. The detailed distribution of the patients and the lesion’s locations are mentioned in Table 2.
Table 1
Age distribution
| Groups | 10-30 years | 31-50 years | 51-70 years | 71 years and above | Mean | Total |
|---|---|---|---|---|---|---|
| Cyst | 12 (30.76%) | 17 (43.58%) | 6 (15.38%) | 4 (10.2%) | 48.23 | 39 |
| Tumour | 1 (0.03%) | 11 (33.33%) | 13 (39.3%) | 8 (24.2%) | 54.87 | 33 |
Table 2
Site distribution
In group A, increased predilection was seen in the case of the maxillary anterior region, at 30.76%, and in group B the posterior mandible, at 48.4%, was seen to be a more common site. The least occurrence was seen with maxillary sinus followed by maxillary posteriors in both groups.
Bone density was calculated by the greyscale measurements taken from the epicentre of each lesion in group A and group B were noted and tabulated to find out the mean range. The maximum average greyscale value was noted for odontogenic keratocyst, with the mean value and standard deviation of 1282 ± 18, while the lowest range of greyscale value was seen for residual cyst, with the mean and standard deviation of 1145 ± 15 (Table 3).
Table 3
Average greyscale values o f group A (cystic lesions)
Table 4 shows the greyscale values of group B, which included the tumour-like lesions; it was found that it showed a higher range of greyscale values with the maximum being the odontome, with the mean and standard deviation being 2138.5 ± 15.5. The mean value with standard deviation for the greyscale values of ameloblastoma and adenomatoid odontogenic tumour were 1369.33 ± 62.5 and 1391.66 ± 64.0, respectively.
Table 4
Average greyscale values for group B (tumour like lesions)
The total range for the greyscale values for cyst was 1117-1303 with the mean value and standard deviation being 1208.375 ± 93, whereas the total range for the greyscale values for tumour was 1117-1303, with the mean value and standard deviation being 1208.375 ± 93.
There was a clear difference in the ranges of the mean greyscale values for cysts and tumours.
Unpaired t test was applied to check if the difference in average greyscale values was significant. The results obtained are shown in Table 5.
Table 5
Comparison between greyscale values of cysts and tumours
| Groups | Average greyscale value | Standard deviation | SE | t value | p value | Remark |
|---|---|---|---|---|---|---|
| Cyst | 1208.375 | 93.0 | 75.5522 | –5.6416 | 0.0001 | Significant |
| Tumour | 1603.000 | 425.5 |
It can be concluded from the above table that there was a significant difference between the average greyscale values of cystic lesions and tumour lesions. This feature may be used to identify the type of lesion, because it is clear from the above-average greyscale values that these values are higher in the case of tumour lesions than those of cystic lesions.
Table 6 shows the different ranges greyscale values in radiopaque, radiolucent, and mixed lesions in cysts and tumour-like lesions.
Discussion
With the advent of radiology, multiple studies have been carried out for the diagnosis and differentiation between different pathologies of the jaw. Odontogenic pathologies closely resemble each other, making it more difficult to differentiate them clinically and radiographically. Since three-dimensional imaging modalities like computed tomography scan (CT scan), magnetic resonance imaging (MRI), and CBCT came into the picture there has been a tremendous increase in the advantages associated with diagnosis and treatment planning. The radiation attenuation in CT imaging of different tissue is calculated in Hounsfield units (HU) thus making it easier to define what a given finding may represent. HU measures the radiodensity on a quantitative scale [1,8]. CBCT introduced for dental use has many advantages such as high resolution acquisition and, compared with conventional CT, lower radiation doses with smaller and less expensive equipment [9]. A large number of studies have shown a linear relationship between Hounsfield units (HU) in CT scans and greyscale in CBCT, which can be used for the estimation of bone density [8,10].
Patrick et al. [11] in the year 2017 evaluated the correlation between Hounsfield units of multislice computed tomography (MSCT) scans and greyscale values in CBCT in various fields of view for hyperdense as well as hypodense structures. It was found that the grey values for hypodense structures in large-volume CBCT scans were more reliable and analogous to Hounsfield units in MSCT. However, for hyperdense structures the grey value of CBCT may not be as accurate as the HU value of a CT scan.
In limited volume CBCT imaging, the attenuation of X-ray beam becomes maximised and minimised at various points in the scan due to the 360° rotation of the CBCT machine for the data acquisition. This phenomenon might in turn reduce the overall density value in the limited imaging volume [8].
Also, the use of anti-scatter grids in CT scans helps to reduce the scattered radiation which cannot be prevented in CBCT. This causes an increased resultant beam hardening effect, partial volume averaging, and under sampling of the images in CBCT scans, due to which a few authors like Armstrong et al. [12] and Miles et al. [13] suggested a negative correlation between Hounsfield units of CT scans and greyscale values of CBCT.
So, in the present study we tried to use the greyscale value for the detection and differentiation of different osseous lesions.
Trope et al. [14] carried out an in-vitro study by subjecting mandibles of human cadavers to CT scan examinations and found that a cyst could be differentiated from a granuloma by this method. A similar in-vivo study was carried out by Juerchott et al. [15] in the year 2018, in which MRI was found to be useful in the differentiation between cyst and granuloma. Mishra et al. [2] reported in their study that, when taking into consideration the exposure parameters and cost, CBCT may be more convenient and suitable than multislice computed tomography for the evaluation of bony lesions of the jaws caused by cysts and tumours.
Greyscale value for determination of the lesion was also carried out on digitalised radiograph by Shrout et al. [5], who in their study compared the greyscale values of cysts and granulomas on a histogram. It was concluded that granulomas had a narrower range and lower greyscale value than cyst.
Results obtained in the study given by Nasim et al. [1] also showed that there is strong correlation of greyscale value that is seen in cases of cysts and tumours which can be attributed to the bone density level and therefore considered as a major diagnostic tool in the branch of dentistry.
The present study was aimed in determining whether the greyscale values depicted in CBCT differentiate different benign osseous lesions of the jaw. Hence, the greyscale values were calculated for the geometric centres of the lesion. In most instances the geometric centre of the lesion contains tissue that is homogenous, i.e. it contains either solid mass of tissue or fluid or air, etc.
Because determining the greyscale value for borders or margins of the lesion was beyond the scope of our study, the greyscale values were not calculated at the margins. We were not able to find any literature addressing the greyscale values for the borders of the lesion, and thus an entirely new study should be planned to assess the greyscale values for the lesion margins and borders.
In the present study, a definitive difference in the ranges of greyscale values between cysts and tumour lesions was noted, with the tumours having a higher range of values when compared to cysts. Thus, the greyscale value can be used as one of the differentiating aids in benign osseous lesion of the jaw.






