CHEST RADIOLOGY / ORIGINAL PAPER
Quantitative assessment of thoracic morphometry in interstitial lung diseases: a CT-based comparison of nonspecific interstitial pneumonia, usual interstitial pneumonia, and healthy control
1
Department of Radiology, Faculty of Medicine, Inonu University, Malatya, Turkey
2
Department of Physiotherapy and Rehabilitation, Faculty of Health Sciences, Erzurum Technical University, Erzurum, Turkey
Submission date: 2025-11-03
Final revision date: 2026-02-02
Acceptance date: 2026-02-03
Publication date: 2026-04-13
Corresponding author
Hilal Er Ulubaba
Department of Radiology, Inonu University, Faculty of Medicine, postcode: 44280, Malatya, Turkey
Department of Radiology, Inonu University, Faculty of Medicine, postcode: 44280, Malatya, Turkey
Pol J Radiol, 2026; 91(1): 179-186
KEYWORDS
TOPICS
ABSTRACT
Purpose:
This study aimed to quantitatively assess thoracic morphometry using thoracic computed tomography (CT) in patients with nonspecific interstitial pneumonia (NSIP), usual interstitial pneumonia (UIP), and healthy controls, and to determine whether morphometric parameters can differentiate between interstitial lung disease (ILD) subtypes.
Material and methods:
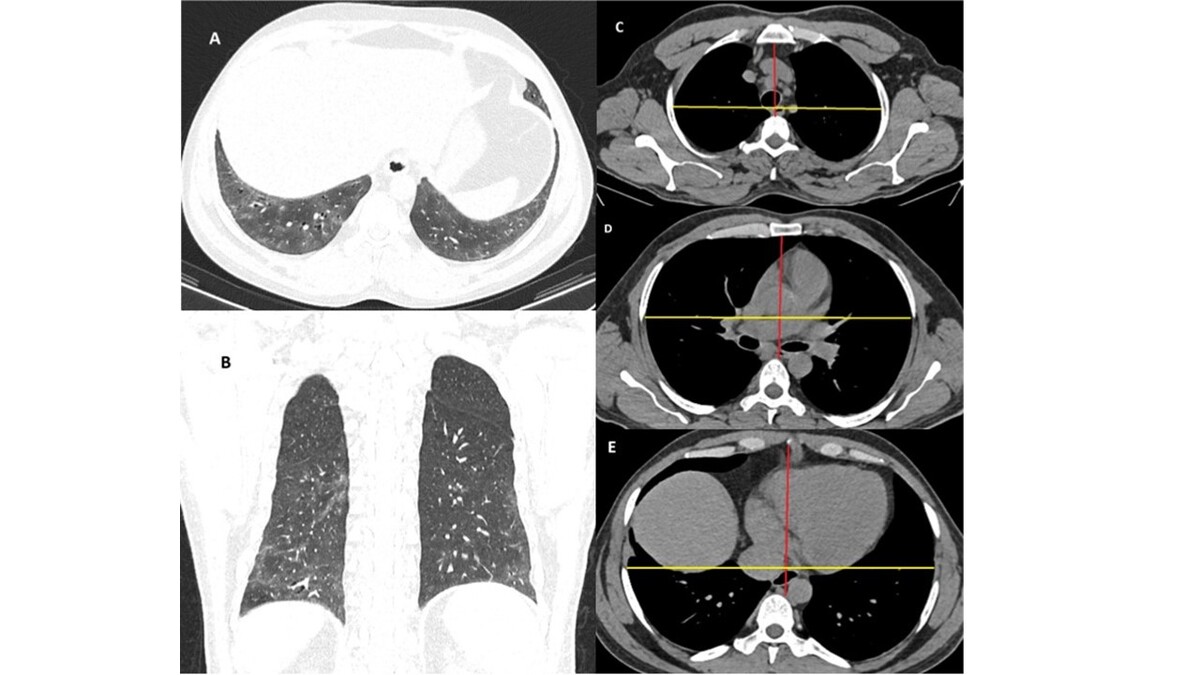
A retrospective, cross-sectional study was conducted involving 180 participants (60 NSIP, 60 UIP, and 60 healthy controls). Standardised thoracic CT scans were analysed at 3 thoracic levels (T3, T6, and T9). The anteroposterior (AP) and transverse (T) thoracic diameters were measured, and their ratios (AP/T) were calculated.
Results:
Significant intergroup differences were observed in thoracic dimensions, mainly at the upper thoracic level (T3). UIP patients showed smaller AP and transverse diameters than NSIP and controls (p = 0.028 and p = 0.003). At T6, the transverse diameter was also reduced in UIP compared with controls (p = 0.029). The AP/T ratio did not differ significantly (p > 0.05), suggesting preserved thoracic geometry despite dimensional reduction. NSIP values were intermediate between UIP and controls.
Conclusions:
Quantitative CT-based thoracic morphometry reveals distinct structural differences among ILD subtypes. Patients with UIP show reduced upper thoracic dimensions consistent with restrictive remodeling, whereas NSIP demonstrates relatively preserved thoracic configuration. CT-derived thoracic diameters represent simple, reproducible, and cost-effective imaging biomarkers that may complement conventional pattern analysis and support objective disease assessment.
This study aimed to quantitatively assess thoracic morphometry using thoracic computed tomography (CT) in patients with nonspecific interstitial pneumonia (NSIP), usual interstitial pneumonia (UIP), and healthy controls, and to determine whether morphometric parameters can differentiate between interstitial lung disease (ILD) subtypes.
Material and methods:
A retrospective, cross-sectional study was conducted involving 180 participants (60 NSIP, 60 UIP, and 60 healthy controls). Standardised thoracic CT scans were analysed at 3 thoracic levels (T3, T6, and T9). The anteroposterior (AP) and transverse (T) thoracic diameters were measured, and their ratios (AP/T) were calculated.
Results:
Significant intergroup differences were observed in thoracic dimensions, mainly at the upper thoracic level (T3). UIP patients showed smaller AP and transverse diameters than NSIP and controls (p = 0.028 and p = 0.003). At T6, the transverse diameter was also reduced in UIP compared with controls (p = 0.029). The AP/T ratio did not differ significantly (p > 0.05), suggesting preserved thoracic geometry despite dimensional reduction. NSIP values were intermediate between UIP and controls.
Conclusions:
Quantitative CT-based thoracic morphometry reveals distinct structural differences among ILD subtypes. Patients with UIP show reduced upper thoracic dimensions consistent with restrictive remodeling, whereas NSIP demonstrates relatively preserved thoracic configuration. CT-derived thoracic diameters represent simple, reproducible, and cost-effective imaging biomarkers that may complement conventional pattern analysis and support objective disease assessment.
REFERENCES (15)
1.
Belloli EA, Beckford R, Hadley R, Flaherty KR. Idiopathic non‐specific interstitial pneumonia. Respirology 2016; 21: 259-268.
2.
Escalon JG, Legasto AC, Toy D, Gruden JF. Central paradiaphragmatic middle lobe involvement in nonspecific interstitial pneumonia. Eur Radiol 2021; 31: 7143-7150.
3.
Jo YS, Lee HK, Park SH, Joh JS, Jang HJ, Park JS. Korean guidelines for diagnosis and management of ıdiopathic nonspecific ınterstitial pneumonia. Tuberc Respir Dis 2025; 88: 237-246.
4.
Mukhopadhyay S. Usual interstitial pneumonia (UIP): a clinically significant pathologic diagnosis. Mod Pathol 2022; 35: 580-588.
5.
Milad N, Esmaeil I, Atefeh A, Mehran M, Mohsen S, Maryam K, et al. Lung ultrasound for assessing disease progression in UIP and NSIP: a comparative study with HRCT and PFT/DLCO. BMC Pulm Med 2025; 25: 11. DOI: 10.1186/s12890-024-03433-8.
6.
Zhan X, Koelsch T, Montner SM, Zhu A, Vij R, Swigris JJ, Chung JH. Differentiating usual interstitial pneumonia from nonspecific interstitial pneumonia using high-resolution computed tomography: the “straight-edge sign”. J Thorac Imaging 2018; 33: 266-270.
7.
Glenn LM, Troy LK, Corte TJ. Diagnosing interstitial lung disease by multidisciplinary discussion: a review. Front Med 2022 (Lausanne); 9: 1017501. DOI: 10.3389/fmed.2022.1017501.
8.
Walsh SL, De Backer J, Prosch H, Langs G, Calandriello L, Cottin V et al. Towards the adoption of quantitative computed tomography in the management of interstitial lung disease. Eur Respir Rev 2024; 33: 230055. DOI: 10.1183/16000617.0055-2023.
9.
Chikasue T, Sumikawa H, Sumi A, Matsumoto K, Murotani K, Tanoue S, et al. Volume histogram analysis of whole-lung CT: differentiating usual from nonspecific interstitial pneumonias and predicting prognosis. Jpn J Radiol 2026; 44: 291-302.
10.
Lim SJ, Kim JY, Lee SJ, Lee GD, Cho YJ, Jeong YY, et al. Altered thoracic cage dimensions in patients with chronic obstructive pulmonary disease. Tuberc Respir Dis 2018; 81: 123-131.
12.
Sadiq IZ, Usman A, Muhammad A, Ahmad KH. Sample size calculation in biomedical, clinical and biological sciences research. J Umm Al-qura Univ Appl Sci 2025; 11: 133-141.
13.
Brixey AG, Oh AS, Alsamarraie A, Chung JH. Pictorial review of fibrotic interstitial lung disease on high-resolution CT scan and updated classification. Chest 2024; 165: 908-923.
14.
Pušeljić M, Mohorko B, Počivavšek T, Moazedi-Fürst F, Schmid J, Fuchsjäger M, Talakić E. Effect of slice thickness on quantitative analysis of interstitial lung disease: a retrospective volumetric chest CT study. Radiol Med 2025; 130: 1172-1182.
15.
Mengesha MG, Meena J, Ramachandran K, Shetty AP, Thippeswamy PB, et al. Correlation analysis between computed tomography and magnetic resonance imaging for assessing thoracic pedicle morphology. World Neurosurg 2023; 180: e599-e606. DOI: 10.1016/j.wneu.2023.09.116.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.